High blood pressure that refuses to budge can feel like an endless loop of new prescriptions and tighter lifestyle rules. If you’re managing blood pressure resistant to multiple medications, you know that small changes often feel like long shots. Dealing with stubborn numbers is exactly why health experts frequently document how higher-sodium eating patterns raise blood pressure risk, especially when convenience meals dominate the diet.
A randomized clinical trial evaluated a practical potassium-enriched salt substitute kitchen swap for this high-risk group. Findings suggest a modest improvement in 24-hour blood pressure monitoring results. Safety experts emphasize a critical factor often missed in summaries: potassium-based salt substitutes are not safe for every health condition.

New Research on Potassium-Enriched Salt Substitutes for Hypertension
Key Findings from the Salt Substitute Clinical Trial
Clinical Evaluation of Salt Substitution in Daily Diet
A clinical randomized trial evaluated a potassium-enriched salt substitute in adults with resistant arterial hypertension over 24 weeks. This study, detailed in the 24-week clinical study of mineral-based salt substitutes, focused on swapping daily salt instead of adding another pill to the patient’s regimen.
Isolating the salt-swap effect from the false swings typical in standard clinical measurements was a core priority of this study design.
The Role of 24-Hour Ambulatory Blood Pressure Monitoring (ABPM)
Ambulatory monitoring, often called ABPM, measures blood pressure throughout the day and night rather than capturing one clinic moment.
Monitoring your numbers throughout the day is vital because blood pressure naturally rises and falls with stress, sleep quality, and caffeine. Even a rushed morning can spike numbers, making single readings less reliable than a full 24-hour snapshot.
Clinicians are prioritizing this trial because resistant hypertension carries extreme cardiovascular risk. When someone is already taking several drugs and the numbers remain elevated, clinicians start looking for additional strategies that are realistic for daily life, including the kind that can happen in a kitchen without turning meals into punishment.
Quick Facts: Potassium Salt Substitutes for Hard-to-Treat Hypertension
These quick facts are meant to answer the first wave of voice-search questions, like “what changed in the salt substitute study” and “is a potassium salt substitute safe for high blood pressure.” They also help separate what was actually tested from what is often implied in viral summaries.
The intervention in this trial utilized a potassium chloride blend to replace sodium chloride, a strategy that continues to show promise in managing stubborn numbers. Research continues to show that dietary adjustments can significantly impact stubborn hypertension numbers.
- Study type: Randomized, double-blind pilot trial in resistant hypertension.
- Duration: 24 weeks of consistent mineral substitution.
- Primary measurement: 24-hour ambulatory blood pressure monitoring.
- Main result: A modest reduction in systolic blood pressure compared with regular salt.
- Safety signal: No clinically significant hyperkalemia reported in the pilot group.
- Important caveat: Pilot study size means results are promising but not definitive.
These findings highlight how minor kitchen swaps can support long-term heart health. While the results are narrow, they provide a measurable strategy for those struggling with hard-to-treat readings.
- Broader context: In the U.S., more than 70% of sodium comes from packaged or restaurant foods, so the biggest wins often start with what is already baked into labels.
While these initial findings offer a promising path for hard-to-treat groups, larger clinical studies must still confirm long-term safety for high-risk patients.
Explaining Trial Results for Patients with Resistant Hypertension
Defining Resistant Hypertension and its Challenges
The Definition People Actually Live With
Resistant hypertension occurs when blood pressure stays above goal despite taking three different medication classes at max doses, usually including a diuretic. Clinicians often rely on a standard definition of resistant hypertension to describe cases where four or more medications are required for control.
Living with this condition is often exhausting. Patients frequently find themselves:
- Taking several different pills every morning and night.
- Sticking to strict grocery lists and low-sodium rules.
- Watching their monitor only to see high numbers stay stuck.
This frustration is common, as the effort put into lifestyle changes doesn’t always show up on the scale or the cuff right away.
Why Clinicians Look for Hidden Pressure Boosters
Resistant hypertension also pushes clinicians to check for extra factors that can sabotage progress, including factors that keep blood pressure high despite treatment, like sleep apnea, certain medications, heavy alcohol intake, and missed doses that happen when life is hectic.
Successes and Limitations of the Salt Substitute Study
What Moved in 24-Hour Blood Pressure
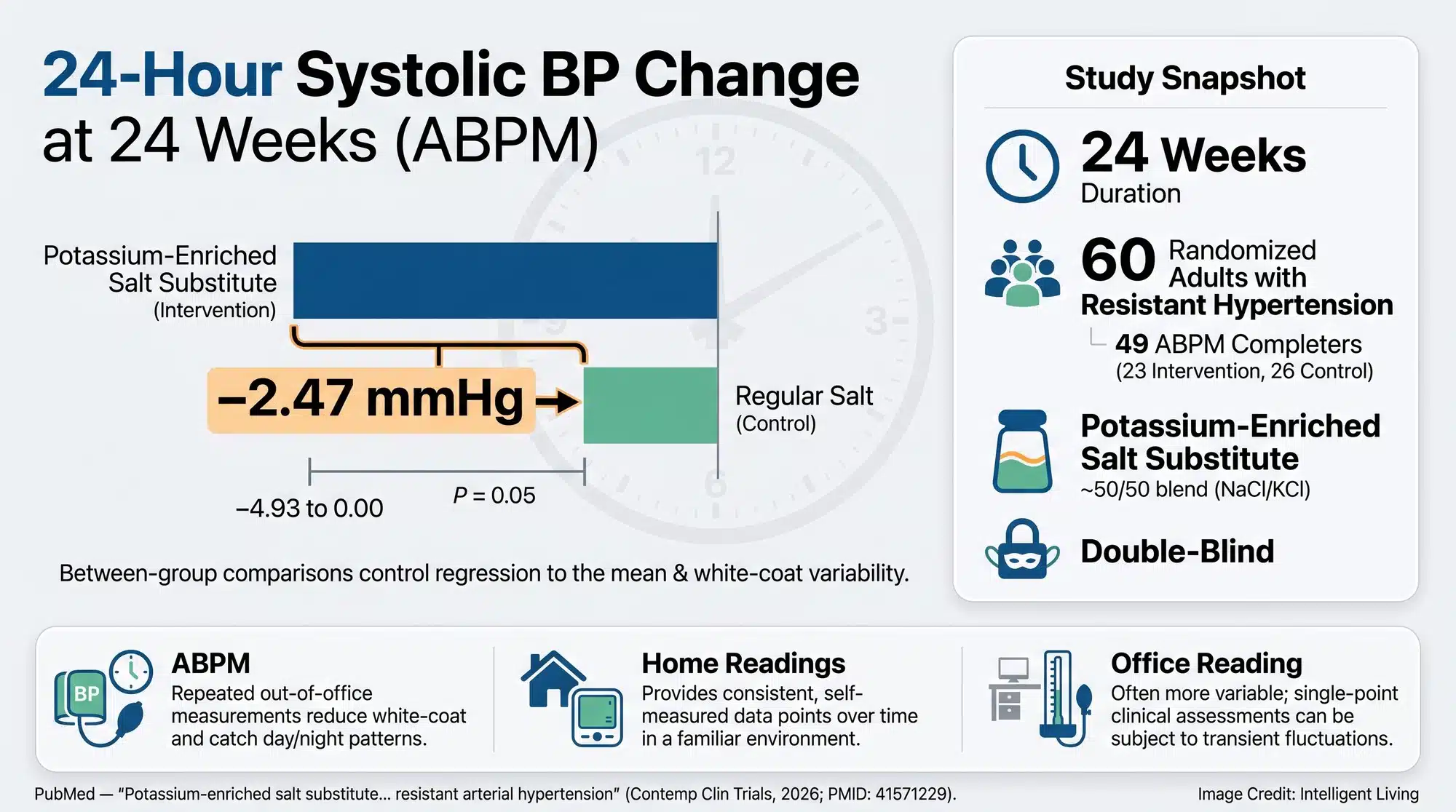
Data from the pilot trial showed that switching to the salt substitute led to a directionally greater drop in 24-hour systolic blood pressure compared to regular table salt. The published abstract reports a between-group difference of about 2.5 mmHg with a borderline statistical result. It also notes that urinary potassium excretion rose in the intervention arm while urinary sodium changes were modest, as captured in the trial’s reported 24-hour blood pressure and urine findings.
Cutting back on salt while eating more potassium shifts how your body handles fluids and relaxes your blood vessels. Lowering sodium while increasing dietary potassium shifts fluid handling and vascular tone, though results vary based on individual physiology and baseline diet.
What the Study Could Not Prove Yet
Focusing on 24-hour monitoring allowed the study to test blood pressure movement rather than long-term heart attack or stroke prevention. Bigger trials are still needed to confirm long-term outcomes, safety in broader risk groups, and whether the effect holds when people use the substitute inconsistently.
Why Out-of-Office Blood Pressure Monitoring Keeps Coming Up
Doctors look at multiple readings because blood pressure changes constantly throughout the day. Common traps like ‘white-coat hypertension’—where numbers spike just because you’re at the doctor’s office—can make it hard to get a true reading.
Because of this, out-of-office blood pressure monitoring using ABPM or home readings is the best way to confirm your numbers before making big changes to your treatment.
A clinical review on interpreting 24-hour cardiovascular signal patterns details how repeated measurements can uncover discordant patterns and why nighttime blood pressure often carries extra signal about cardiovascular risk.

Safety Guidelines and Global Standards for Potassium Salt Substitutes
Contraindications: Who Should Not Use Potassium Salt Substitutes
Why Potassium can Turn from Helpful to Hazardous
Potassium-based salt substitutes typically replace part of sodium chloride with potassium chloride. Potassium is essential for nerve signaling and healthy heart rhythm, but too much potassium can become dangerous when the body cannot clear it efficiently.
Potassium concentration varies wildly between products, often delivering a surprising dose per teaspoon that can overwhelm reduced kidney function. Delivery of high potassium chloride concentrations can happen surprisingly fast, overwhelming the system when kidney function is reduced or medication combinations raise potassium levels.
An overview of electrolyte substitution risks and benefits emphasizes that overall population benefits depend on protecting high-risk groups.
Where Kidney Function Changes the Math
For those living with chronic kidney disease, the warning is blunt. Specialists emphasize that potassium chloride seasonings can be risky in chronic kidney disease. Even a routine-looking renal health indicator panel can suggest that potassium clearance is already dangerously tight.
Who Can Consider vs. Who Should Ask a Clinician First
| Group | General Guidance |
|---|---|
| Adults with normal kidney function and no high-risk medications | May consider modest substitution after a medical check-in |
| People with chronic kidney disease | Should avoid or use only under close medical supervision |
| Those taking potassium-sparing diuretics or certain blood pressure medications | Require clinician guidance and may need lab monitoring |
| Individuals with adrenal or severe heart conditions affecting potassium balance | Medical supervision strongly advised |
Why it Worked for Them but Not for Me is Often a Measurement Trap
Blood Pressure is a Moving Target
Your numbers are rarely fixed; they bounce based on your sleep, stress, and even how much water you’ve had. Research into blood pressure response variability suggests many apparent successes or failures are actually artifacts of short monitoring windows.
Short Trials Create False Stories
A salt substitute started during a week of deadlines and five-hour nights can look “useless,” while the same swap started during a calmer month can look dramatic. Dehydration triggers, like salty travel meals or long flights, create mild shifts that tilt your readings and confuse the true story of your heart health.
World Health Organization (WHO) Standards for Salt Substitutes
Discretionary Salt Versus Packaged Sodium
International standards for mineral-based salt alternatives suggest replacing table salt with lower-sodium versions in general populations, while excluding people with kidney impairments or other circumstances that could compromise potassium excretion.
Global recommendations focus on discretionary salt added during cooking rather than the hidden sodium engineered into packaged foods.
Why Ultra-Processed Defaults Matter
Ultra-processed foods often bake sodium into the shopping cart before anyone reaches for a salt shaker, a pattern broken down by sodium engineered into many products, a risk associated with ultra-processed foods that requires careful label monitoring. When grocery aisles feel like a second language, identifying ultra-processed labels through the NOVA framework makes dietary trade-offs clearer without turning eating into a chore.

Future Implications for Food Standards and Clinical Care
Emerging Trends in Hypertension Management
- Expect clinicians to discuss potassium-enriched salt substitutes more frequently with patients whose blood pressure stays high despite taking several medications.
- Public health messaging may place more emphasis on discretionary salt reduction while continuing to push for packaged-food sodium reductions.
- Expanding the FDA proposal that permits salt substitutes in standardized foods may soon allow manufacturers to reformulate packaged products for lower sodium levels.
- Larger trials may test whether modest shifts in 24-hour blood pressure translate into fewer strokes and heart attacks.
- Home blood pressure devices and apps may increasingly nudge people toward structured measurement routines when diet changes are made.
- Patients who previously dismissed salt substitutes as ineffective may reconsider once they understand how much day-to-day variability can distort short trials.
- A large SSaSS salt substitution trial linked salt substitution with a significant reduction in strokes, moving the strategy from the kitchen to public health.
A newer synthesis also suggests details matter, using a comparative analysis of mineral blends to examine differences in sodium and potassium concentrations.
Safe Implementation Guide for Home Salt Substitution
Build a Baseline Before You Change Anything
Establish your starting point by recording measurements at the same time daily for two weeks, providing a reliable average for clinical review. Measuring blood pressure at the same time each day for one to two weeks gives a clearer starting point than a few scattered readings. Many people only notice patterns after a few days of consistent checks, like numbers that run higher after short sleep or after back-to-back salty meals.
Get the Measurement Technique Right
How you measure your blood pressure is just as important as how often you check it. An automatic upper-arm cuff is usually your most dependable option.
To get the most accurate reading, make sure you are following proper home measurement protocols:
- Sit quietly and rest for a few minutes before starting.
- Ensure the cuff is placed correctly on your bare arm.
- Take two separate readings about a minute apart and average them.
Getting the steps right ensures that simple errors don’t make your numbers look higher than they actually are.
Make the Swap Gradual and Watch for the Real Signal
Try a partial substitution first instead of jumping to a full switch. Taste adapts over time, and gradual change can make the habit stick while giving blood pressure time to show whether the average is truly shifting.
Know When a Clinician Should Be in the Loop
Anyone with kidney disease, conditions that affect potassium balance, or medications that raise potassium should treat this as a clinician-guided decision. In real-world care models, structured home hypertension management can turn scattered numbers into actionable clinical patterns.
Finally, interpret changes over weeks, not days. A single low or high reading does not define success or failure. Patterns matter more than isolated spikes.

Salt Substitute and Resistant Hypertension: What this Means for Long-Term Heart Health
Pilot findings suggest that potassium-enriched salt substitutes offer a helpful tool for managing resistant hypertension. While this swap is easy for many to try, it works best when combined with broader lifestyle changes.
If you are managing blood pressure that resists multiple drugs, remember these core takeaways:
- Incremental shifts matter: Small drops in your numbers can significantly lower your long-term risk.
- Medication is still key: This kitchen swap supports your prescriptions rather than replacing them.
- Safety comes first: Respecting safety boundaries and avoiding high-potassium risks is vital.
The biggest challenge is staying consistent while ignoring the noise of day-to-day spikes.
Some researchers are also exploring device-based approaches for drug-resistant cases, including ultrasound pulses delivered to renal nerves, though most people manage through diet and habit.
Common Questions About Salt Substitutes and Blood Pressure
How does a potassium salt substitute lower blood pressure?
Potassium-enriched salt lowers blood pressure by correcting your sodium-to-potassium balance, allowing kidneys to flush excess fluid more efficiently.
Is a potassium-enriched salt substitute safe for everyone?
No. People with chronic kidney disease (CKD), those on potassium-sparing diuretics, or individuals with heart conditions must consult a doctor first to avoid dangerous potassium buildup.
Can I use salt substitutes if I have kidney disease?
Kidney specialists generally advise against them. Because the kidneys clear excess potassium, impaired function can lead to hyperkalemia, a high-potassium state that affects heart rhythm.
How long does it take for a salt swap to show results?
You should interpret changes over several weeks rather than days. Blood pressure is noisy and bounces daily, so you need a consistent 24-hour blood pressure monitoring routine to see a true trend.
Do salt substitutes taste different than regular salt?
Most people notice a slight metallic or bitter aftertaste if used in large amounts. Mixing it gradually with regular salt can help your taste buds adapt while still reducing your overall sodium intake.
